Researchers from a tertiary orthopedic center in India have detailed a series of patients who experienced latent reactivation of osteoarticular tuberculosis (OATB) in the knee, highlighting a clinical pattern that can elude early detection. The cases, published in Cureus, underscore that even after successful pulmonary treatment, Mycobacterium tuberculosis may linger in joint tissue and reactivate months to years later, causing chronic knee pain, swelling and joint destruction.
Key Findings from the Case Series
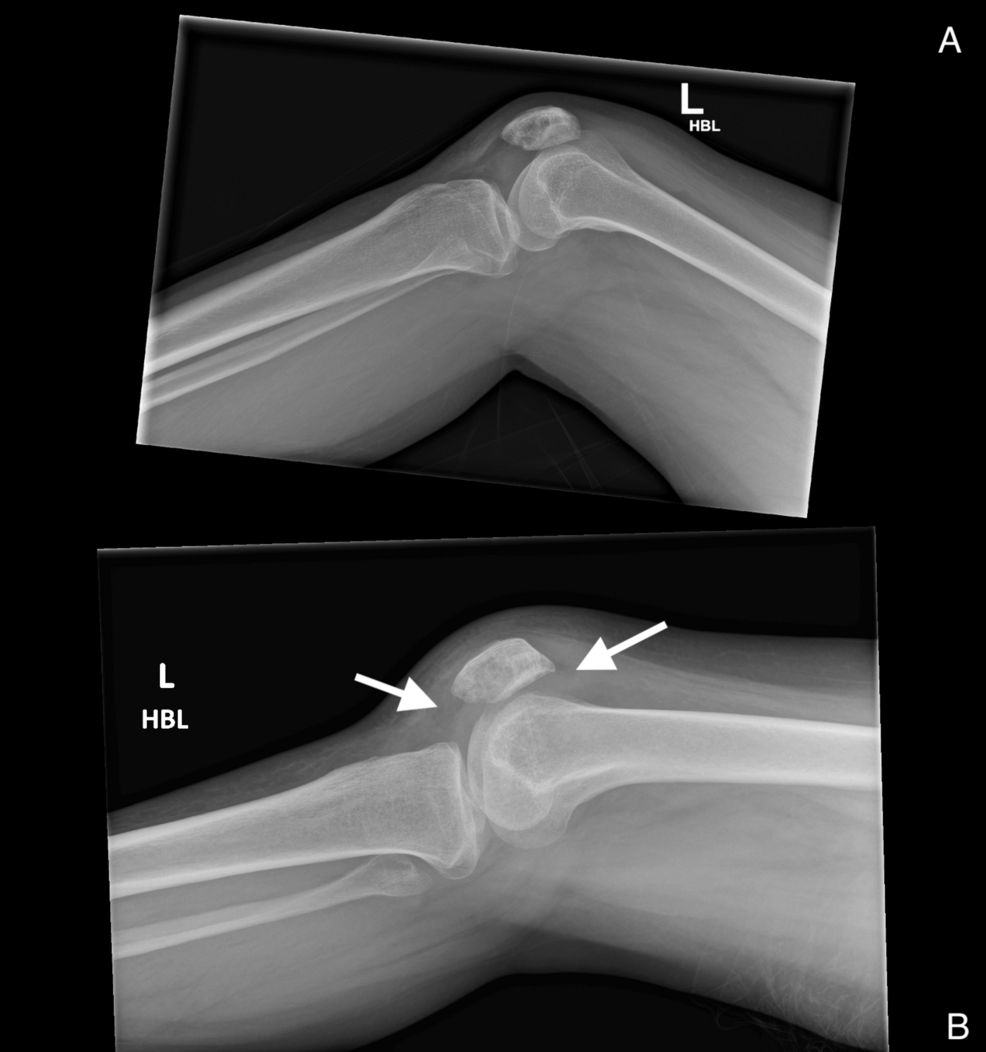
The authors described five adults, ages 22 to 58, who presented with progressive knee effusion and limited range of motion despite prior treatment for pulmonary TB. Each patient had been declared sputum‑negative and completed a standard six‑month regimen at least 12 months before joint symptoms began. Magnetic resonance imaging (MRI) showed synovial hypertrophy, marrow edema in the distal femur and proximal tibia, and peripheral rim‑enhancing collections—findings that align with the imaging patterns described in recent radiology reviews of OATB.
Microbiological confirmation was achieved in four patients through polymerase chain reaction (PCR) testing of synovial fluid, while histopathology revealed caseating granulomas in all five. Treatment consisted of a 12‑month course of first‑line anti‑tubercular drugs (isoniazid, rifampicin, pyrazinamide, ethambutol) plus adjunctive physiotherapy. All patients achieved clinical remission, though three required arthroscopic debridement to restore knee function.
Clinical Context and Epidemiology
Osteoarticular tuberculosis accounts for roughly 1 % to 3 % of all TB cases worldwide, according to the World Health Organization’s Global Tuberculosis Report 2023. Of this small subset, spinal involvement (Pott’s disease) dominates, representing about half of OATB, while peripheral joints such as the knee comprise roughly 30 % of extra‑spinal disease. A systematic review of 573 patients with native‑joint TB found an overall recurrence rate of about 7 %, indicating that reactivation after apparently successful treatment is not rare.
Risk factors that predispose to latent joint infection include HIV co‑infection, diabetes mellitus, chronic steroid use, and prior extrapulmonary TB. In regions with high TB burden, delayed diagnosis is common because knee TB mimics common degenerative or inflammatory arthritides, leading to an average diagnostic delay of 12 to 24 months in many series.
Diagnosis: Imaging and Laboratory Advances
Early MRI is now regarded as the modality of choice for detecting subtle marrow changes and synovial disease before radiographs show erosions. Characteristic MRI signs—multiple vertebral‑like involvement of adjacent bone, preservation of disc space, and rim‑enhancing abscesses—help distinguish TB from pyogenic infections, which typically have thicker, irregular walls. The imaging spectrum described by Jangid et al. in 2024 corroborates these features and emphasizes the value of diffusion‑weighted sequences for assessing treatment response.
Laboratory confirmation remains essential. While culture is the gold standard, it can take six to eight weeks. GeneXpert MTB/RIF and line‑probe assays provide rapid detection of Mycobacterium tuberculosis DNA and rifampicin resistance, with sensitivity exceeding 80 % in extrapulmonary specimens. In the Cureus series, PCR of synovial fluid yielded a positive result in 80 % of cases, underscoring its clinical utility.
Treatment Strategies and Public‑Health Implications
Current WHO guidelines recommend a minimum of nine months of therapy for skeletal TB, extending to 12 months for complex cases or when drug resistance is suspected. The Cureus cohort followed a 12‑month regimen, reflecting real‑world practice where clinicians opt for longer courses to safeguard against relapse, especially in weight‑bearing joints.
From a public‑health perspective, latent joint TB poses a silent reservoir that can fuel transmission if undiagnosed. In low‑incidence countries like the United States, bone and joint TB represent less than 1 % of all TB cases, yet the CDC warns that delayed diagnosis increases the risk of disability and healthcare costs. Strengthening awareness among primary‑care physicians and orthopedists is therefore a priority, as early imaging and molecular testing can curtail the need for extensive surgical reconstruction.
Future Directions in Research and Care
Ongoing trials are evaluating shorter, all‑oral regimens that include newer agents such as bedaquiline and delamanid for multidrug‑resistant bone TB. Host‑directed therapies, including vitamin D supplementation and adjunctive interferon‑γ, are being studied for their potential to enhance microbial clearance and reduce inflammation.
Clinicians are encouraged to maintain a high index of suspicion for TB in any chronic mono‑articular knee effusion, especially in patients with a history of pulmonary disease or immunosuppression. Prompt MRI, coupled with rapid molecular diagnostics, can secure an early diagnosis and allow for organ‑preserving treatment.
For readers seeking more detailed guidance on osteoarticular TB, see the CDC’s clinical overview of bone and joint TB. Read more on Globally Pulse Health for updates on emerging TB therapies and public‑health strategies.